Surgeon Operated With IV in Foot for 18-Hour Brain Surgery
Surgeon IV in foot during brain surgery — not a headline anyone expected to be real. But the photograph is real: a glucose line snaking across a sterile floor, a foot vein doing the work a forearm couldn’t, and six inches away, a man in surgical gloves still operating on an open human brain. The image didn’t go viral because it’s shocking. It went viral because it’s true in ways the healthcare system would prefer to keep quiet.
Eighteen hours in, Dr. Yuksel Yilmaz collapsed beside the operating table at a hospital in Istanbul, Turkey. Blood sugar crashed. Nurses moved fast. He refused to stop. So they threaded a glucose drip into a vein in his foot — the only part of him that didn’t need to stay sterile — and he kept going. The question the photograph doesn’t answer: what does a choice like that cost?

When the Surgeon’s Body Becomes the Emergency
Hypoglycemia — the clinical term for dangerously low blood glucose — doesn’t announce itself politely. According to the American Diabetes Association, blood sugar below 70 mg/dL triggers sweating, confusion, and trembling. Below 54 mg/dL, the brain begins to malfunction. Dr. Yilmaz didn’t collapse because he was careless. He collapsed because he had, by all accounts, simply not eaten in nearly a full day. Neurosurgeons operating on complex cases routinely restrict their own fluid and food intake during long procedures — not out of stubbornness, but because leaving a patient’s open skull to use a restroom introduces infection risk, breaks surgical flow, and, in some critical moments, simply isn’t survivable for the patient. Hypoglycemia can escalate to seizure and unconsciousness within minutes if untreated.
Dr. Yilmaz was already there.
What the nursing team did next is the part of this story that deserves its own examination. They didn’t call a halt. They didn’t page a replacement surgeon — in Turkey’s public hospital system, there often isn’t one standing by for a case this specialized. Instead, they improvised with precision: a peripheral IV line, glucose solution, a foot vein. The logic is clean. Hands must stay sterile; feet don’t need to be. It’s the kind of field improvisation that rarely gets documented. This time, someone had a camera.
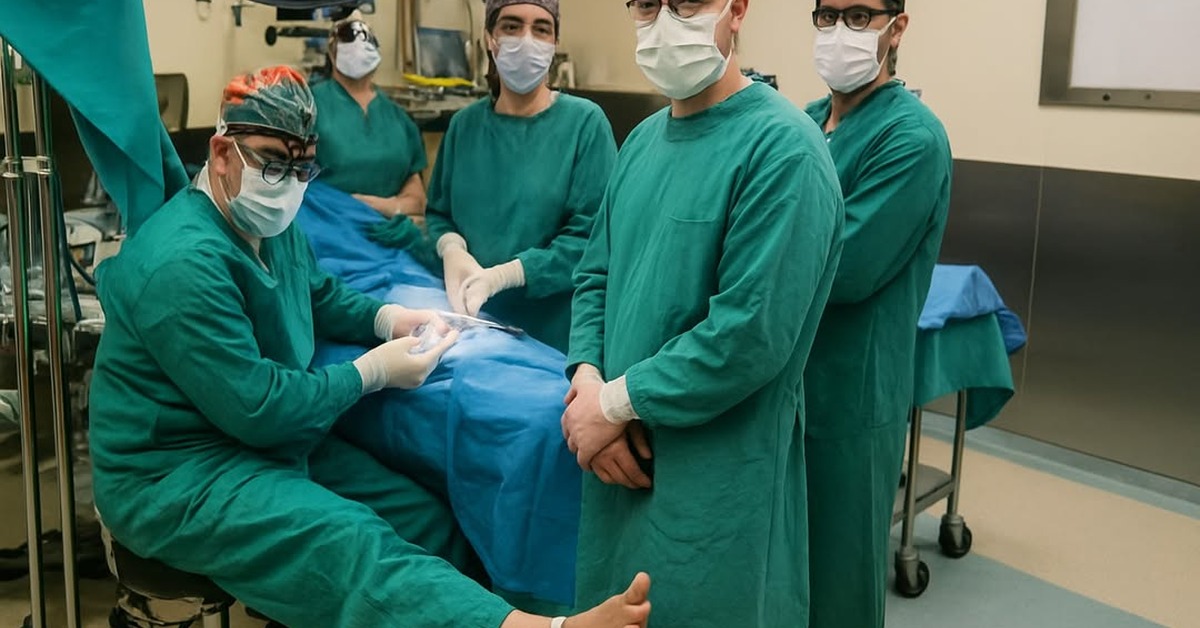
His posture, in the photograph, is exhausted. Dr. Yilmaz sits on a stool, hunched slightly, the IV line coiling across the floor like something out of a war documentary. His gaze is locked on the surgical field. The patient’s skull was still open. Theater staff present that day confirmed his focus never wavered.
What Marathon Surgery Actually Demands of a Human Body
Why does this matter? Because the physical cost of long surgical procedures is rarely discussed outside occupational medicine journals, and even more rarely attached to a real name and a real face.
Neurosurgery sits at the extreme end of medicine’s physical demands — and not just because of the brain’s complexity. Duration does most of the damage. Challenging cranial procedures — removal of deep-seated tumors, repair of arteriovenous malformations, multi-stage aneurysm clipping — routinely run between 6 and 15 hours. Surgeons stand, or hold their arms in sustained positions, for the entirety. Orthopedic strain accumulates in the lower back, shoulders, and neck at rates that would alarm any occupational health specialist. A 2019 study by researchers at the University of Michigan found that surgeons performing procedures longer than six hours showed measurable deterioration in fine motor precision in the final hours — the very hours that often contain the most delicate work.
Stories like Dr. Yilmaz’s exist alongside a quieter epidemic of physician burnout and injury that rarely makes international headlines. For a parallel look at how medical improvisation saves lives under impossible constraints, consider the story of a baby operated on before she was even born — another case where the limits of what medicine can do were redrawn in real time.
Turkey’s public health infrastructure adds another layer. According to OECD Health Statistics 2023, Turkey has approximately 1.9 practicing physicians per 1,000 people — well below the OECD average of 3.7. For a subspecialty as narrow as neurosurgery, the gaps are even starker. In major urban centers like Istanbul, a single neurosurgeon may carry caseloads that would constitute a staffing crisis in Western European systems. Dr. Yilmaz’s refusal to abandon his patient wasn’t only personal devotion. It may also have been, in the coldest practical sense, the only real option. The hospital has not released the patient’s name or detailed diagnosis, citing privacy. What Turkish media confirmed is simpler: the surgery was ultimately successful. The patient survived.
The Global Crisis Behind One Photograph
Here’s the thing — this story didn’t go viral simply because it’s dramatic. It went viral because it confirmed something people already suspected about medicine: that the system’s most extraordinary outcomes are often quietly paid for by the people inside it. Physician burnout is not a new phenomenon. The World Health Organization classified it as an occupational syndrome in 2019, citing exhaustion, cynicism, and reduced professional efficacy as its hallmarks. But healthcare workers have documented the physical cost of long surgical shifts for decades.
A landmark 2011 study in the Archives of Surgery found that surgeon fatigue significantly increased the risk of self-reported medical errors, particularly in procedures lasting beyond eight hours. The surgeon IV in foot during brain surgery image that erupted across social media this week gave that statistic a face — no longer an abstract percentage, but a man on a stool with a glucose drip snaking across a sterile floor, still looking at the brain he hasn’t finished saving. BBC Future’s investigation into healthcare burnout found that the emotional and physical toll on frontline medical workers constitutes one of the least-addressed public health crises of the 21st century.
What makes Dr. Yilmaz’s case particularly striking is that it inverts the usual narrative. We’re accustomed to stories about system failure — patients harmed because an exhausted surgeon made an error. This is the opposite: a surgeon IV in foot during brain surgery, remaining lucid enough, steady enough, committed enough to carry a procedure across the 18-hour mark without catastrophe. That’s not evidence that the system works. It’s evidence that certain individuals absorb what the system fails to provide — and the system has quietly learned to depend on that.
The distinction matters enormously if you’re trying to fix anything. Hospitals across Europe, North America, and parts of Asia have begun implementing mandatory rest protocols for surgical teams in recent years. The European Working Time Directive limits junior doctors to 48-hour work weeks. Senior surgeons frequently operate outside those protections. The reforms are real, but they’re also incomplete — and in underfunded public hospital systems, they can be close to theoretical.
A Surgeon IV in Foot: What the Image Reveals About Medicine’s Hidden Bargain
Medical ethics has a concept called the duty to treat — the implicit obligation a physician accepts when a patient is in their care and no adequate alternative exists. It’s not absolute. Formal limits exist in both international and national medical law. But inside an operating theater where a patient’s skull is open and the only available neurosurgeon has just collapsed, abstract ethics compress into a single question: do I stop?
And that compression, it turns out, has a measurable neurological basis. A 2020 analysis by researchers at Harvard Medical School, published in the Journal of the American Medical Association, examined cases of physician self-sacrifice during extended emergencies and found a consistent pattern: surgeons who continued operating under severe personal duress reported, in retrospective interviews, a narrowing of conscious attention so complete that their own physical symptoms registered as secondary information (researchers actually call this attentional tunneling under duress). Not ignored. Secondary. The brain, it seems, is capable of a kind of clinical triage on itself.
That finding reframes what we’re looking at in the Istanbul photograph entirely. Dr. Yilmaz wasn’t heroically suppressing pain through willpower alone — his neurology was doing something measurable, deprioritizing proprioceptive signals, flooding the prefrontal cortex with task-specific focus, running the body on borrowed glucose while keeping the hands steady. It is, in a precise and unsettling way, the brain saving itself by saving someone else’s. The IV in his foot wasn’t just a medical intervention. It was a negotiation between two bodies — one open on the table, one folded on a stool — with a surgeon serving as the only bridge.
The surgical team in Istanbul deserve specific recognition here. The nurses who improvised the foot IV didn’t do so randomly. Peripheral venous access in a non-standard site requires clinical judgment about vessel viability, flow rate, and solution compatibility. They made a fast, correct call. Medicine runs on those calls. It just rarely photographs them. A world that treats this image purely as a human-interest story is missing the institutional diagnosis embedded in it.
How It Unfolded
- Late 20th century: Marathon neurosurgical procedures — some exceeding 12 hours — become standard for complex tumor removal and vascular repair as imaging technology advances, raising questions about surgeon endurance for the first time.
- 2003: The Accreditation Council for Graduate Medical Education in the United States caps surgical resident work hours at 80 per week, acknowledging the first formal link between surgeon fatigue and patient safety risk.
- 2011: Research published in the Archives of Surgery documents measurable increases in medical error rates during procedures exceeding eight hours, shifting the conversation from anecdote to data.
- 2025: Dr. Yuksel Yilmaz completes an 18-hour brain surgery in Istanbul with a glucose IV threaded into his foot, and the image circulates globally, forcing the question of what institutional reform has actually changed.
By the Numbers
- 18 hours: confirmed duration of Dr. Yilmaz’s surgery before the IV intervention became necessary
- 70 mg/dL: the blood glucose threshold below which the American Diabetes Association classifies hypoglycemia as clinically dangerous
- 1.9 physicians per 1,000 people: Turkey’s practicing physician ratio (OECD Health Statistics, 2023), compared to an OECD average of 3.7
- 48 hours: the maximum weekly working hours for doctors under the European Working Time Directive — a limit that doesn’t cover senior surgeons in many member states
- 6–15 hours: the typical duration range for complex cranial procedures, including deep tumor removal and arteriovenous malformation repair, according to neurosurgical literature
Field Notes
- Foot veins are among the least commonly used sites for peripheral IV access in adults — flow rates are slower than forearm veins, and patients can’t walk with a line there. The Istanbul nursing team’s choice was unusual and entirely deliberate: it was the only site that kept the surgeon’s hands free and sterile simultaneously.
- Surgeons performing long procedures routinely wear compression garments to reduce deep vein thrombosis risk — the same risk that IV access in a lower limb increases. The nursing team was, in effect, managing competing medical risks in real time.
- Turkey has one of the highest rates of medical tourism in the world, with Istanbul’s major hospitals attracting patients from across the Middle East, Central Asia, and Eastern Europe. Structural pressure on specialist surgeons there is categorically different from that in countries where medical tourism is minimal.
- Researchers still can’t definitively answer whether a surgeon at hour 16 or 18 is statistically more dangerous than one at hour 1 — because ethics boards won’t approve studies that deliberately induce that level of fatigue in controlled conditions. The data we have comes almost entirely from retrospective self-reporting, which introduces its own distortions.
Frequently Asked Questions
Q: What exactly happened to the surgeon IV in foot during brain surgery — and was it medically safe?
Dr. Yuksel Yilmaz collapsed beside the operating table after approximately 18 hours of surgery, likely due to severe hypoglycemia. His nursing team inserted a peripheral IV line into a foot vein and administered a glucose drip while he remained at the surgical field. It’s an unconventional access site but not inherently unsafe — peripheral IVs in foot veins are clinically valid, though less common. The intervention stabilized him sufficiently to complete the procedure.
Q: How do surgeons typically manage food and hydration during extremely long operations?
It’s a system that works until it doesn’t. Many surgeons minimize fluid intake for hours before a long procedure specifically to avoid needing bathroom breaks, which interrupt sterile conditions and surgical momentum. Caloric preparation — eating a solid meal beforehand — is standard practice, but in emergency or unplanned extended cases, that window can close fast. Some hospitals now have protocols for team rotations or brief supervised pauses, but implementation varies enormously by institution and resource level.
Q: Does surgeon fatigue actually increase the risk of mistakes, or is this overstated?
It’s not overstated, but it’s more nuanced than “tired surgeons make more errors.” A 2011 study in the Archives of Surgery found that surgeons self-reported significantly higher rates of errors during procedures over eight hours. But experienced surgeons also develop compensatory strategies — slower movements, more deliberate checking — that partially offset fatigue effects. The honest answer is that the risk is real, it’s measurable, and the degree to which it manifests depends heavily on individual experience, case complexity, and team support. Dr. Yilmaz’s case doesn’t resolve that question. It makes it harder to ignore.
Editor’s Take — Dr. James Carter
What unsettles me most about this story isn’t the image itself — it’s what the image normalizes. We’re calling Dr. Yilmaz’s choice heroic, and it is. But heroism at this scale is also a symptom. When the only way to finish saving a patient is to treat yourself through a foot vein on a stool, the system has already failed. The courage is real. So is the institutional gap that made it necessary. We should be able to hold both of those things at once — and feel uncomfortable that we can’t seem to fix the second one.
Medicine, at its edge, looks nothing like the version we see in television dramas or hospital brochures. It looks like a glucose drip coiling across a sterile floor. It looks like a man on a stool who has been standing, in every meaningful sense, for 18 hours. Dr. Yilmaz’s patient went home. That outcome is real, and it matters. But somewhere in another operating theater in another underfunded hospital in another city whose name you won’t see trending, another surgeon is making the same calculation — quietly, without a camera, without an IV in their foot yet. What happens when they run out of ways to improvise?